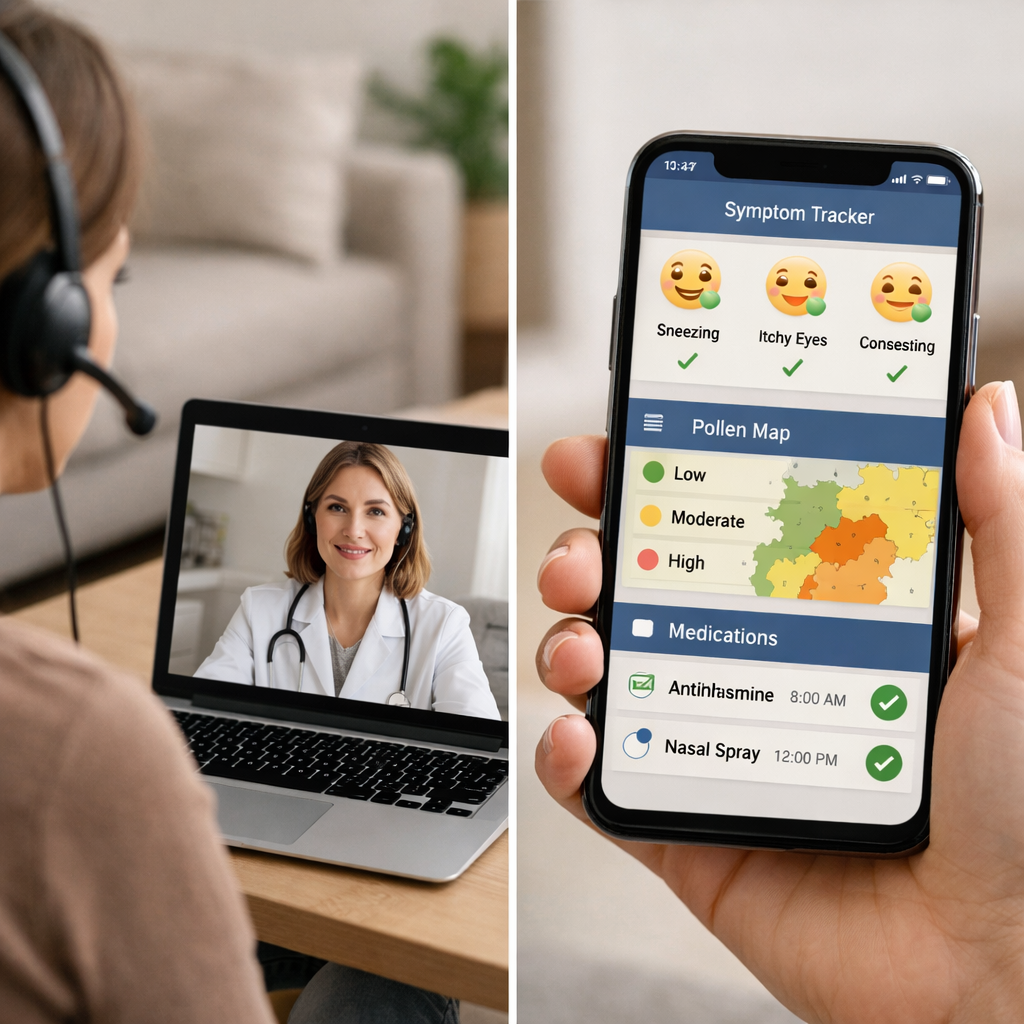
Telehealth Allergy Care vs. Apps: Which Platform Works Best?
Telehealth and allergy apps aren’t rivals—they solve different problems. If you need diagnosis, prescriptions, or a treatment plan, choose a virtual allergy doctor through telehealth. Use apps to stick to that plan: track symptoms, set medication reminders, and time your day around pollen peaks. In allergy care, they work best together. Clinicians report high comfort using telehealth for follow-ups—97% in one specialty case study—and virtual care has remained a meaningful part of allergy and asthma practice post‑peak adoption (AMA telehealth in allergy case study). For families aiming for clear, cost‑aware control, start with a clinical plan via telehealth, then let a great app help you follow it. Too Allergic helps you compare options and prepare for each step.
Quick answer and how to choose
Use telehealth for medical decisions; use apps to make those decisions stick day to day. Telehealth handles diagnosis, prescriptions, and care planning; apps deliver tracking, reminders, and exposure alerts. Most follow-ups can happen virtually, with strong clinician acceptance and ongoing use in allergy care (AMA telehealth in allergy case study).
“Telehealth allergy care” is real-time or asynchronous virtual visits with licensed clinicians who assess symptoms, prescribe medications like second-generation antihistamines and intranasal steroids, adjust treatment plans, and coordinate tests; it complements in‑person evaluation for procedures requiring equipment, such as skin testing or pulmonary function assessments.
Quick chooser:
- Symptoms likely needing meds or a diagnosis → telehealth (online allergy treatment).
- Daily monitoring, med reminders, and adherence → app.
- Considering immunotherapy (SLIT) or unclear triggers → telehealth plus targeted in‑person tests.
- Severe or rapidly worsening symptoms (trouble breathing, throat swelling) → in-person/urgent care.
What telehealth allergy care includes
A typical virtual visit covers the same decision‑making you’d expect in clinic:
- Live video or phone with a board‑certified clinician.
- E‑prescriptions sent to your local pharmacy (Doctor On Demand allergy care).
- Step‑by‑step workflow: create account → complete intake/history → visit → e‑prescription and plan → follow‑up or triage to in‑person testing when needed.
Common prescriptions include second‑generation antihistamines (cetirizine, loratadine, fexofenadine, levocetirizine), intranasal steroids (fluticasone/Flonase, triamcinolone/Nasacort), and intranasal antihistamines (like azelastine). Expect modern platforms to offer secure messaging, scheduling, and visit summaries, with pharmacy connections to reduce delays. Too Allergic’s telehealth comparisons note which services support these basics.
What allergy apps do well
Apps shine between visits. The best help you remember and record:
- Medication reminders, refill tracking, and adherence streaks.
- Symptom diaries and shareable logs for your clinician.
- Local pollen alerts and peak times to guide outdoor plans.
- Barcode scanning for food risk awareness and grocery decisions (allergy management apps roundup).
Quality varies. A review of 48 allergy‑related apps reported a mean MARS score of 3.31±0.43/5, and many lacked clinician‑developed action plans—use them to support, not replace, medical guidance (Frontiers in Allergy review). Helpful examples: MyTherapy and Medisafe (free reminders, tracking), Tally (simple symptom tallies, Apple Watch), Pollen.com Allergy Alert (neighborhood pollen), ShopWell (barcode scanning). Too Allergic highlights app features that support adherence and communication with your clinician.
Decision criteria for allergy platforms
Use this short checklist:
- Clinical scope: diagnosis, prescriptions, and virtual allergy doctor access.
- Cost model: per‑visit vs subscription; transparent fees; insurance acceptance.
- Access: 24/7 coverage, urgent versus specialty care, Spanish support when needed.
- Pediatric readiness: dosing guidance, family scheduling, school forms.
- Security: HIPAA compliance, encryption, clear data policies.
- Integrations: pharmacy e‑prescribe; EHR connectivity for continuity.
Evidence notes: telehealth reduces no‑shows and supports chronic disease management; security is a top concern—favor reputable, HIPAA‑compliant platforms with clear privacy controls (virtual allergy care overview). Blend telehealth with targeted in‑person testing when triggers are unclear or immunotherapy is on the table (Frontiers in Allergy review). Too Allergic uses this checklist in side‑by‑side reviews to help you choose faster.
Side-by-side comparison
| Dimension | Telehealth | Apps |
|---|---|---|
| Diagnosis and care planning | Can diagnose many clear‑symptom cases remotely and build a care plan; triages to testing when needed. | Cannot diagnose; organizes symptoms and exposures to inform clinical decisions. |
| Prescriptions and pharmacy access | E‑prescribes most non‑controlled allergy meds; often same‑day pickup; many services offer 24/7 access. | No prescribing; tracks doses, refills, and side effects to improve adherence. |
| Ongoing monitoring and adherence | Ideal for dose adjustments, side‑effect checks, and plan updates; widely accepted for follow‑ups. | Best for daily logs, reminders, and pollen alerts; quality varies across apps (MARS ≈3.3/5). |
| Costs, insurance, and value | Transparent per‑visit fees; many plans cover telehealth; broad platform maturity and investment. | Mostly free or low‑cost; value depends on reminders, logs, and data export/sharing. |
| Privacy and data control | Choose HIPAA‑compliant platforms with encryption and clear privacy policies. | Privacy standards vary; review permissions and data‑sharing settings carefully. |
| Pediatric suitability and safety | Pediatric dosing, non‑drowsy options, and school action plans via virtual visits. | Family reminders, shared symptom logs; does not replace clinician dosing advice. |
| When in-person testing is needed | Orders skin tests or lung function tests and coordinates hybrid care. | Helps track patterns that point to which tests are needed. |
Diagnosis and care planning
Many common, clear‑symptom conditions can be accurately diagnosed remotely, with a personalized care plan and follow‑up triage when tests are necessary (GoodRx telehealth overview). A care plan is a tailored set of treatments—medications, avoidance steps, and follow‑up intervals—adjusted over time as symptoms and risks change. Virtual care cannot perform skin or lung function tests; hybrid models fill the gap (Frontiers in Allergy review).
Prescriptions and pharmacy access
Telehealth can prescribe most non‑controlled allergy medications, including steroid nasal sprays, with visit costs often $0–$99 depending on insurance (Doctor On Demand allergy care). E‑prescriptions typically route to your local pharmacy, and major platforms frequently offer 24/7 access and broad specialty coverage (GetStream telemedicine roundup). Apps don’t prescribe; they keep you on schedule and flag refills.
Ongoing monitoring and adherence
Use apps for daily symptom logs, dose reminders, and exporting trends to your clinician; diary quality varies (MARS ≈3.31/5) (Frontiers in Allergy review). Schedule telehealth follow‑ups for dose changes, side‑effect checks, and action‑plan updates—clinicians report very high willingness to manage follow‑ups virtually (97%) (AMA telehealth in allergy case study). Add local pollen alerts to time outdoor activities.
Costs, insurance, and value
Representative pricing: LiveHealth Online urgent/allergy visits around $55; Teladoc near $75 per visit; MDLIVE urgent care up to $82 and mental health up to $284; MDBox from $59 (GetStream telemedicine roundup). Coverage varies by insurer and plan (GoodRx telehealth overview). The telehealth market is projected to grow from $87.4B in 2025 to $286.4B by 2032, underscoring platform maturity (telemedicine market projections). Too Allergic’s comparisons summarize cost structures and coverage considerations to clarify trade‑offs.
Privacy and data control
Pick HIPAA‑compliant telehealth platforms with secure video, encrypted messaging, role‑based access, and clear audit trails (top telehealth software features). Security remains a leading concern; mitigate risk by choosing reputable services and reviewing privacy settings. For apps, inspect permissions, data sharing, and export options before you start logging.
Pediatric suitability and safety
For kids and adults, favor non‑drowsy, second‑generation antihistamines (cetirizine, loratadine, fexofenadine, levocetirizine) and pediatric‑approved intranasal steroids (fluticasone, triamcinolone) when appropriate. Confirm age ranges, dosing, and sedation profiles during telehealth visits. Use family‑friendly apps for shared reminders and symptom logs to bring into virtual check‑ins.
When in-person testing is needed
In‑person care is needed for skin prick or intradermal testing, pulmonary function testing, or evaluation of severe or rapidly worsening symptoms. A hybrid approach—telehealth plus targeted clinic visits—works well for comprehensive evaluation and immunotherapy planning, with high patient satisfaction; one UK series found 85% rated non‑face‑to‑face allergy visits good or very good (Frontiers in Allergy review).
Pricing and access snapshot
- LiveHealth Online: about $55/visit; 24/7 access; Spanish support available on major platforms (GetStream telemedicine roundup).
- Teladoc: around $75/visit; 24/7 access (GetStream telemedicine roundup).
- MDLIVE: urgent care up to $82; mental health up to $284; 24/7 access (GetStream telemedicine roundup).
- MDBox: from $59 (GetStream telemedicine roundup).
- Doctor On Demand: $0–$99 with insurance, $99 uninsured; can prescribe steroid nasal sprays and other non‑controlled meds (Doctor On Demand allergy care).
- Hybrid immunotherapy programs: example pricing around $99/month with supervised first dose and at‑home maintenance (virtual allergy care with in‑person visits).
Use Too Allergic’s comparison to see how these options line up by price, access, and scope.
Recommendations by common goals
Fast symptom relief on a budget
Use a lower‑fee telehealth platform (~$55–$82) for rapid assessment and same‑day prescriptions when appropriate. Consider OTC non‑drowsy antihistamines first‑line; add an intranasal steroid if congestion dominates. Use a free app (MyTherapy or Medisafe) for reminders and to track your response.
Non-drowsy daily control for kids or adults
Prioritize second‑generation antihistamines and pediatric‑appropriate intranasal steroids. Confirm age approvals and dosing in a telehealth visit, then log daily symptoms in an app and export weekly summaries for virtual follow‑ups; most clinicians are comfortable managing follow‑ups by telehealth (AMA telehealth in allergy case study). Add pollen alerts to reduce exposure.
Nasal-first approach for congestion
Start with a daily intranasal steroid; consider adding an intranasal antihistamine if needed. Telehealth can prescribe steroid nasal sprays. Pair with saline rinses, then recheck via telehealth in 2–4 weeks using your app logs to guide dose changes.
Long-term control with SLIT tablets or drops
Sublingual immunotherapy (SLIT) places allergen tablets or drops under the tongue to build tolerance; FDA‑approved tablets exist for select allergens. Expect first‑dose supervision for at least 30 minutes, a very low anaphylaxis risk (on the order of 1 in 100 million), early improvements in 4–8 weeks, and about 3 years for durable benefit, with programs typically around $99/month, HSA/FSA‑eligible (virtual allergy care with in‑person visits). Use telehealth to assess fit, then confirm triggers with in‑person testing.
Mixed or unclear triggers needing testing
Start with telehealth to prioritize likely triggers and order tests. Track symptom timing, environments, and exposures in an app before your clinic visit; share logs to refine the skin‑test panel or decide on pulmonary function testing (Frontiers in Allergy review).
How to blend telehealth and apps for better outcomes
Try this five‑step loop:
- Telehealth intake and baseline plan.
- App‑based symptom and adherence tracking.
- Telehealth follow‑up to optimize meds.
- Targeted in‑person testing if needed.
- Long‑term monitoring with periodic virtual checks.
Benefits include fewer no‑shows, flexible scheduling, and stronger chronic‑disease control; prioritize HIPAA‑compliant platforms for security (virtual allergy care overview). Blended care combines virtual visits, high‑quality apps, and selective in‑person testing to maximize access and control.
Safety notes and what telehealth cannot do
Telemedicine cannot perform skin testing or pulmonary function tests; use a hybrid plan when these are needed (Frontiers in Allergy review). Seek urgent, in‑person care for breathing difficulty, throat or tongue swelling, severe wheeze, or signs of anaphylaxis. Too Allergic offers research‑driven, non‑medical guidance to help you prepare for informed conversations with licensed clinicians.
Too Allergic’s take
Start with telehealth for timely, budget‑aware relief and a personalized plan; layer in reputable apps for adherence and pollen awareness. When triggers are uncertain or immunotherapy is considered, blend virtual visits with targeted testing. We favor non‑drowsy options for kids and adults, nasal‑first strategies for congestion, and transparent SLIT timelines, costs, and safety. For deeper comparisons, see our telehealth allergy platform comparison at Too Allergic.
Frequently asked questions
Can a telehealth visit diagnose allergies without testing?
Often, yes—especially when symptoms are clear. Too Allergic can help you prepare questions for that visit.
Will a telehealth provider prescribe non-drowsy antihistamines or nasal steroids?
In many cases, yes, with e‑prescriptions sent to your local pharmacy. Too Allergic outlines which platform features support straightforward prescribing.
Are allergy apps accurate and safe to use for daily decisions?
Apps are helpful for reminders, symptom logs, and pollen alerts, but they don’t replace medical advice. Too Allergic recommends using them to support your plan and share data with your clinician.
How do I know if my child’s allergy is appropriate for virtual care?
If symptoms are stable and non‑urgent, a telehealth visit can review history, dosing, and school plans. Too Allergic can help you prep for that conversation.
When should I skip virtual care and go in person or urgent care?
Go in person for severe symptoms like breathing difficulty, throat swelling, or suspected anaphylaxis, and when your clinician recommends skin testing or lung function testing. Too Allergic is not a medical provider and does not replace emergency care.