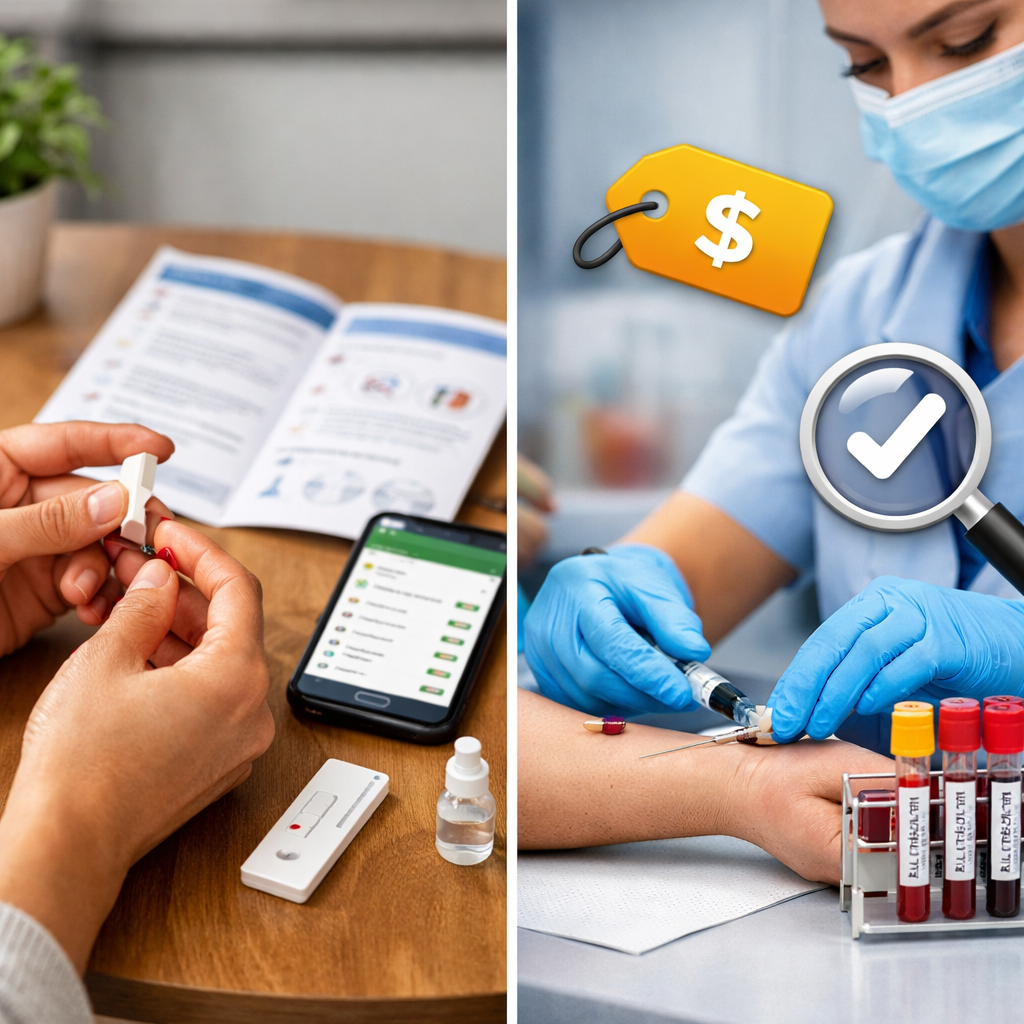
At-Home Allergy Tests vs Lab Testing: Accuracy, Cost, Convenience
Choosing between at-home allergy tests and clinician-directed lab testing comes down to three things: accuracy and clinical value, total cost, and convenience. The short answer: consumer kits can be a useful first look—especially for environmental triggers—but they are not designed to diagnose allergies or guide treatment on their own. Clinician-ordered testing and interpretation remain the safest path to confirm true allergy, particularly for foods, where missteps can put nutrition and safety at risk. If a home kit suggests a concern, bring the results to a licensed clinician before changing your diet or care plan. Too Allergic helps families decide when a home screen is reasonable and what to confirm in clinic.
| Feature | At-home kits | Clinician-directed testing |
|---|---|---|
| Where sample is collected | At home | Clinic or clinical lab |
| Sample type | Finger-prick blood; sometimes saliva or hair | Skin testing in office; venous blood for lab |
| Biomarkers measured | Often IgE panels for environmental allergens; many “food sensitivity” kits measure IgG | Specific IgE (blood), skin prick test wheal size; oral food challenge confirms |
| Turnaround time | Typically days (often ~5 business days after lab receipt) | Same-day for skin tests; days for bloodwork; scheduled challenges |
| Who interprets | Self-service portal; sometimes brief telehealth consult | Allergy specialist integrates results with history |
| Accuracy/validation | Variable; IgG food kits are not diagnostic | Validated methods with quality controls |
| What results can/can’t do | Screen and generate hypotheses; cannot confirm allergy | Diagnose, risk-stratify, and plan treatment |
| Typical next step | Confirm positives with a clinician | Begin evidence-based management (e.g., avoidance, meds, immunotherapy) |
What at-home tests are and how they work
Most at-home allergy test kits are direct-to-consumer mail-in services. You collect a small finger-prick blood sample, seal it, and mail it to a lab—some route to CLIA-certified facilities—with results posted to a portal, often within about five business days of lab receipt, according to a Healthline overview of at-home allergy tests (Healthline). Many kits focus on environmental panels (e.g., dust mites, pollens, pet dander). By contrast, a large share of “food sensitivity” offerings measure IgG, not IgE, which means they do not diagnose true food allergy (Healthline).
Direct-to-consumer (DTC) allergy test — A mail-in kit that lets you collect a small sample (usually finger-prick blood; some advertise saliva or hair) at home and view results online without an in-person clinic visit.
Set expectations: home results can help you narrow hypotheses—especially for everyday triggers—but any result that affects safety or diet should be confirmed with a clinician before you act.
What clinician-directed lab testing includes
Clinician-directed allergy care uses validated tests and applies them in context:
- Skin prick test: tiny amounts of allergens are applied to the skin; wheal size helps estimate the likelihood of allergy when interpreted with history.
- Serum specific IgE: a blood test performed in CLIA-certified labs that quantifies IgE directed at individual allergens.
- Oral food challenge: a supervised, stepwise feeding in clinic that definitively confirms or rules out a food allergy when appropriate.
These tools work best together. Blood IgE numbers and skin wheals are informative but require expert interpretation alongside your story to avoid over- or under-diagnosis; coverage for in-office testing is common but varies by plan and referral. For test modalities and the role of food challenges, see this Thermo Fisher Scientific overview contrasting food sensitivity tests and true allergy testing (Thermo Fisher Scientific).
Biomarkers explained IgE vs IgG
IgE: An antibody linked to immediate, classic allergy. When specific IgE binds an allergen, it can trigger rapid symptoms—hives, wheeze, vomiting, even anaphylaxis. Clinicians use skin prick testing and specific IgE blood tests, interpreted with history, to estimate the likelihood of true allergy and decide on next steps.
IgG: An antibody more associated with exposure and, in some cases, tolerance development than with allergy. Elevated food-specific IgG does not diagnose food allergy and is often clinically insignificant; multiple allergy societies do not endorse IgG food testing. As one review notes, IgG levels may simply reflect that you ate the food (MyBetterHealth).
Many over-the-counter IgG “food sensitivity” kits are not FDA cleared, while clinician-ordered allergy blood tests used in medical practice are FDA cleared and part of validated clinical pathways (Thermo Fisher Scientific).
Accuracy and clinical value
The bottom line: at-home results are generally less thorough and can be misleading compared with an allergist’s testing plus interpretation (Healthline). Independent validation for consumer kits is limited; one prominent provider cites 70%–90% accuracy for certain environmental panels, but these figures do not equate to a diagnosis without clinical correlation (PremiumAllergy). In medical settings, skin testing and specific IgE correlate best with clinical allergy when read in context, and a supervised oral food challenge is the definitive confirmation.
Two common pitfalls:
- False positives from broad panel testing when there’s no matching history can misclassify sensitization as allergy; large panels run without a proper story can be wrong 50%–90% of the time (Healthline).
- Variable quality control in consumer testing can add noise that a clinician would otherwise filter through exam and history.
Test types at a glance:
| Test type | Biomarker/measure | Typical validation | Who interprets | Clinical use case | Next step if positive |
|---|---|---|---|---|---|
| At-home environmental screen | Specific IgE (limited panel) | Variable; limited independent validation | Consumer; sometimes brief telehealth | Hypothesis generation for rhinitis/asthma triggers | Clinical confirmation and treatment plan |
| At-home “food sensitivity” kit | IgG to foods | Not diagnostic for allergy | Consumer | Not recommended for diagnosing food reactions | Seek clinician guidance; avoid diet changes until evaluated |
| Specific IgE blood test (lab) | Quantitative allergen-specific IgE | FDA cleared; validated | Allergy clinician | Estimate likelihood of IgE-mediated allergy | Consider skin testing or challenge based on history |
| Skin prick test | Immediate wheal response | Validated in clinic | Allergy clinician | Rapid, in-office assessment | Correlate with history; consider challenge |
| Oral food challenge | Objective clinical reaction | Gold standard | Allergy clinician | Definitive confirmation/rule-out | Formal diagnosis; nutrition and safety plan |
Cost signals and real-world value
Sticker price isn’t the whole story. Consumers may spend $100–$300+ on home kits; some bundle a short consult, but they don’t include a full diagnostic workup or ongoing care. Clinician-directed testing is often partly covered by insurance and includes interpretation, risk assessment, and access to treatments such as immunotherapy, though coverage varies by plan and referral. Value means:
- Accuracy sufficient to guide safe decisions
- Access to treatment pathways (e.g., inhalant immunotherapy, epinephrine training)
- Nutrition counseling that prevents unnecessary restriction, especially for kids Too Allergic’s resources help you weigh total value—not just price—before you buy or book.
Convenience and access
Home kits win on logistics: collect at home, mail the sample, and view results within days (many report about five business days from lab receipt) (Healthline). Some offer finger-prick screens for dozens of common environmental triggers and may include a brief clinician consult.
If you want convenience without compromising clinical rigor, consider telehealth allergy care: a virtual visit can triage whether you need lab IgE testing, skin prick testing, or a supervised challenge and help you avoid unnecessary panels. Explore our patient-centered checklist for telehealth allergy features and virtual clinic comparisons:
- Too Allergic: Essential telehealth features for allergy management
- Too Allergic: Top-rated virtual allergy clinics
Risks, false reassurance, and over-restriction
- IgG-driven “food sensitivity” reports can prompt broad eliminations that risk nutrient gaps without improving symptoms; IgG often reflects exposure, not disease (MyBetterHealth).
- Quality control for some at-home tests is variable, increasing the chance of false positives that mislead families or create anxiety (Lee Health).
- Avoid fringe methods such as pulse testing or hair analysis; they lack validation and can divert you from effective care (PremiumAllergy).
When each option makes sense
- Mild, non-urgent curiosity about environmental triggers: a limited at-home IgE screen can surface hypotheses; confirm anything actionable with a clinician before changing meds or environment.
- Food reactions or immediate symptoms (hives, swelling, vomiting, breathing changes): skip IgG “sensitivity” kits. Seek clinician evaluation for specific IgE and/or skin testing, with a supervised oral food challenge when indicated (ACAAI guidance on home food allergy testing).
- Complex cases (eczema flares, asthma, multiple foods, growth concerns): prioritize allergist-directed testing and coordinated care.
If any at-home result is positive, confirm with a licensed provider before changing your diet or treatment.
Parent-advocate guidance from Too Allergic
- Keep a simple symptom diary—what you ate, exposures, timing, and severity. It’s gold for clinical interpretation.
- Protect nutrition: avoid broad eliminations based on IgG results; get dietitian support for kids and anyone with weight loss or restricted intake.
- For environmental symptoms, pilot small, low-risk changes (e.g., dust-mite covers, HEPA filter) while awaiting clinical input.
- Medical disclaimer: Too Allergic is an independent educational resource. Always consult a licensed clinician for diagnosis and treatment.
Practical recommendation
Use at-home kits to narrow hypotheses—never to make safety-critical decisions. Confirm abnormal or actionable findings with a clinician using specific IgE testing, skin prick testing, and, when appropriate, a supervised oral food challenge before altering diet or treatment. For a deeper look at options, see Too Allergic’s comparison of leading at-home blood allergy tests.
Three steps to act today:
- Identify your main symptom and timing (immediate vs delayed).
- If you try a home kit, choose IgE-focused environmental screens; don’t rely on IgG to diagnose food allergy.
- Book a clinician visit to interpret results and map a confirmed next step.
Frequently asked questions
Are at-home allergy tests reliable enough to diagnose a food allergy?
No—most home “food sensitivity” kits measure IgG, which reflects exposure and doesn’t diagnose true allergy; confirm with clinician-directed IgE/skin testing and, when needed, a supervised oral food challenge. Too Allergic’s checklists can help you prepare for that visit.
What is the most accurate way to confirm an allergy?
Validated IgE testing (skin prick or specific IgE blood tests) interpreted with your history, with a supervised oral food challenge as the definitive confirmation when appropriate. Too Allergic’s guides explain what to expect.
Do bigger skin test wheals or higher IgE numbers mean a more severe reaction?
Not necessarily. Larger wheals or higher IgE suggest a higher likelihood of allergy, not reaction severity; Too Allergic’s resources outline how clinicians interpret results with your history.
Can I try an elimination diet based on an at-home result?
Avoid broad eliminations based solely on at-home results, especially IgG. Too Allergic offers guidance on discussing changes with your clinician or dietitian.
When should I see an allergist instead of relying on a home kit?
If symptoms are immediate, reproducible, or involve breathing, hives, swelling, or suspected food triggers, see an allergist for validated testing and a safe diagnostic plan. Too Allergic’s telehealth and clinic comparisons can help you find care.